Our personal tragedy and determination to overcome COVID-19
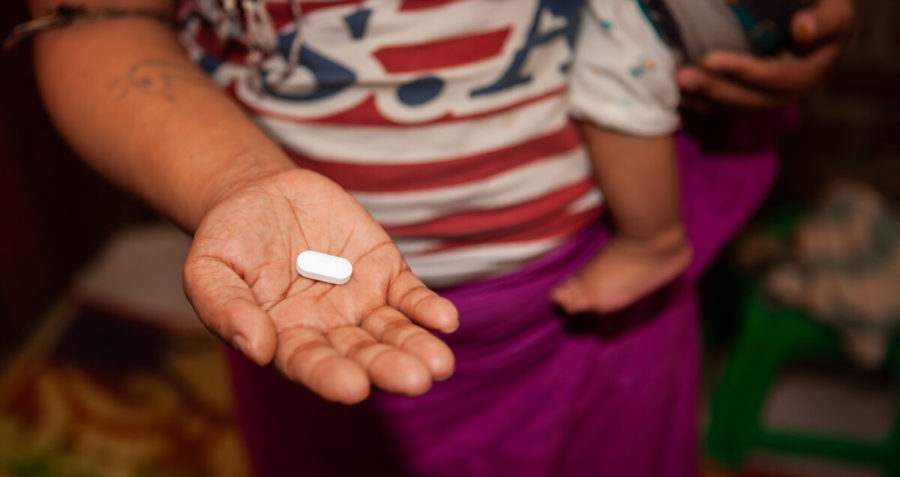 Frontline AIDS/Gemma Taylor/2018
Frontline AIDS/Gemma Taylor/2018
As the second wave of COVID-19 engulfs India, Alliance India is getting critical help to the frontline of the HIV response.
For all of us in India, the second wave of the coronavirus pandemic has created an almost unimaginable crisis. Just as we begin to leave eight months of lockdown, the entire country is being poleaxed. Our public health facilities were unprepared for the speed and severity of the virus and have quickly become overwhelmed.
The situation is delaying critical support to people living with HIV and we are constantly rethinking our approach. We’ve had so many challenges to face, with disrupted communications, limited access to services and lockdown travel restrictions. We’ve also had personal tragedy, with several outreach workers and the head of one of our partner organisations dying from COVID-19.
At Alliance India, we are more determined than ever to support marginalised communities affected by HIV through these impossible times. We are responding to the ever-changing demands of the crisis, in part through the support of a Frontline AIDS’ Accelerating Innovation grant.
India is not prepared to tackle the second wave of COVID-19
The World Health Organisation has classified the variant responsible for the second wave in India as a “variant of global concern,” and preliminary studies have shown it may be more transmissible. India is also suffering from a lack of national coordination as the response is being managed state by state but the state governments aren’t stopping the spread. Add in local elections and festivals that bring populations together without consideration of safe behaviour, and the situation is increasingly desperate.
On top of this, the government booking system for vaccinations cannot cope with the tens of millions trying to book their jabs. Vaccine, treatment and oxygen levels are critically low across the country, despite being the world’s biggest producer of vaccines. And the market rules in India have changed, meaning vaccine prices are likely to significantly increase.
There has also been a historic lack of government spending on health care – just 2% of GDP – and this current catastrophe is the result.
Those living at the edge are impacted the most
Because of societal prejudice, many transgender people, sex workers, men who have sex with men and people living with HIV live below the poverty line with low levels of literacy and education. It’s almost impossible to implement the basic public health and hygiene that’s needed to prevent the spread of COVID-19 in the slums where many of the people we work with live and work. Washing hands, wearing masks and social distancing are not understood to help and so not practiced.
Currently, hospitals can only take in COVID-19 patients and emergencies. Along with the travel restrictions, it makes it much harder for people living with HIV to access their antiretroviral drugs (ARVs). There is genuine anxiety for a person needing to take a vaccine, anxiety that is heightened when they already have a compromised immune system.
Within the communities we work, income has fallen dramatically. It’s getting harder to buy the food needed to take ARVs safely, and stay healthy to fight the effects of HIV. Many people from these communities will not have the ID cards that are essential for the government booking portal to get a vaccine.
There is a lack of guidance on treatment protocols for people living with HIV and COVID-19. It’s making a tough situation much worse because we know discrimination within the healthcare system leads to marginalised people being reluctant to follow their HIV treatment plans. The same could well be true when it comes to take-up of the COVID-19 vaccine.
Supporting innovation to rethink essential service delivery
During the pandemic we’ve needed to move fast and keep flexible, adapting as the virus adapts, to support marginalised people. We’re learning from existing projects and best practices, adapting health programmes and using community structures to raise awareness and understanding within communities. Starting from April, through the Accelerating Innovation grant, funded by Elton John AIDS Foundation, we have begun to strengthen community-based support systems. We’re providing COVID-19 services to the people living with HIV and other communities we work with, alongside linking those most impacted by HIV and COVID-19 to existing care, support and protection schemes.
We’re hoping the pilot project can show us how best practice from HIV programmes can help build the best response to the COVID-19 pandemic for the communities we work with. If successful, we want to replicate and scale up what we’ve learnt to help define the response for the wider population living below the poverty line. And even though we’re in the eye of the storm for wave two of the pandemic, the project must prepare us for any future pandemics.
For this first stage of the project, the priority is to reach 4,000 people from key population groups who are most affected by HIV and others from the wider population. This includes rickshaw pullers, taxi drivers, slum dwellers, unskilled construction labourers and family members.
Fighting adversity on every level
Priorities are constantly shifting, which is another challenge. Increasing COVID-19 testing is urgent, but has to compete with helping individuals register and pay for their vaccinations. Demand is so much higher than we ever expected and we’re caught in the dilemma of who to prioritise. We need to constantly evolve what we have to do, and find the skills to identify, plan and deliver new services.
However hard each day is, the innovation grant has come at the right time, because innovation is enabling us to keep working. For example, through our partner, Gujarat State Network of People living with HIV/AIDS (GSNP+), we’re getting vital services to marginalised people, which we simply wouldn’t be able to do without the grant.
We took direct action as soon as COVID-19 hit. During the first wave, we successfully worked with the treatment centres at state level to ensure three months of ARV medication can be available at one time, cutting down the amount of travel and exposure for clients who usually have to go every month. Even though the work enabled by the innovation grant is just beginning, we’re determined the impact we make will be just as vital to the people we work with.
We will always keep working but we need more support
There is so much we need to do to ensure marginalised communities aren’t left behind in the COVID-19 response, and through this grant we hope to learn lessons and formulate our plans for future responses. Knowing what worked during the first wave puts us in a strong position for the future, so we can help those we work with to keep accessing services without further disruption.
It’s also giving us the opportunity to adapt our services, even through these toughest of times. However severe the crisis becomes, it will never stop our work. We will continue supporting marginalised people, ensuring testing and vaccines are received and completed, and more and more people are aware of and understand the severity of COVID-19.
No-one knows exactly when the second wave will subside, or what the lasting impact will be on marginalised communities. The grant is essential to our work today, and is helping us prepare for the future. But we desperately need more donors to understand the reality of what’s happening on the ground right now in India, and come forward to play their part. We need vital funds to keep our frontline workers supporting the most vulnerable people through the horrors of the pandemic.
We are in curfew mode but we are determined to continue caring for the communities we work with. This is what matters the most and together, we shall overcome.
If you would like to show your support, you can donate funds to Alliance India.
Pemu Bhutia is the Assistant Manager: Institutional Engagement at Alliance India, Thota Maheshwari is the Senior Programme Officer: Sexuality, Gender and Rights at Alliance India.

