New programme aims to reduce new Hepatitis C infections
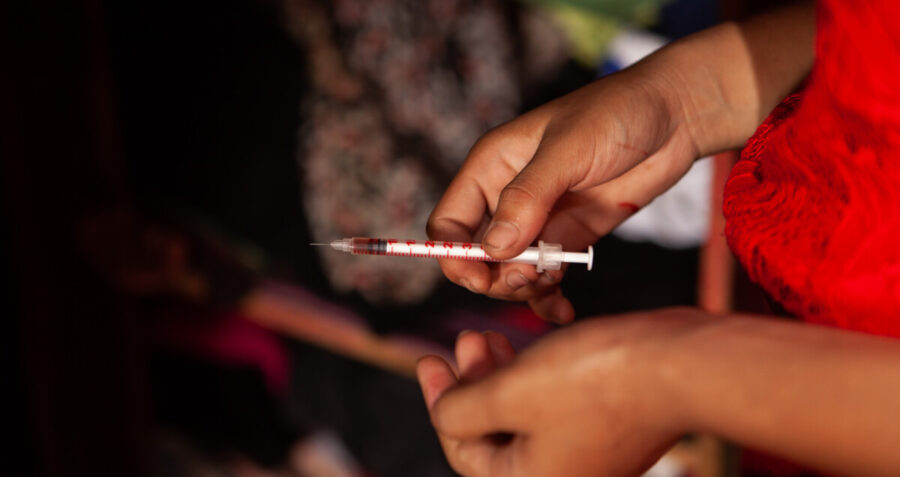 ©Frontline AIDS/Gemma Taylor/2018
©Frontline AIDS/Gemma Taylor/2018
A new three-year programme will build evidence of effective hepatitis C treatments and increase the uptake and scale up of community-led programmes to reduce Hepatitis C infections in three countries.
The programme, led by Frontline AIDS, with funding from UNITAID, aims to reduce new hepatitis C infections amongst people who use drugs in Egypt, Kyrgyzstan and Nigeria. The innovations made through this new programme called ‘Innovate, involve, inspire: Preventing hepatitis C through community-led harm reduction’ could significantly reduce the transmission of hepatitis C and HIV.
Hepatitis C is an inflammation of the liver caused by the hepatitis C virus (HCV). The bloodborne virus can cause both acute and chronic hepatitis, ranging in severity from a mild illness to a serious lifelong illness, including liver cirrhosis and cancer. Infection can occur through exposure to blood from unsafe injection practices, unsafe health care, unscreened blood transfusions, injection drug use and sexual practices that lead to exposure to blood.
According to WHO, globally, an estimated 58 million people have chronic HCV infection. About 1.5 million new infections occurring every year with 80% of these in low- and middle-income countries. HCV disproportionately impacts marginalised populations, people who use drugs and people living with HIV. Antiviral medicines can cure more than 95% of people with hepatitis C infection, but access to diagnosis and treatment is low. While there is currently no effective vaccine against hepatitis C, it is preventable.
We have the tools to prevent new hepatitis C infections. This new programme will put communities at the forefront, building evidence of effective hepatitis C treatments and how new technologies and community-led outreach can improve health outcomes for people who use drugs.Revati Chawla, Interim Head of Programmes, Frontline AIDS
Partners in Egypt, Kyrgyzstan and Nigeria will research the effectiveness and acceptability of under-used hepatitis C prevention innovations with people who use drugs. These include:
- Providing Long-Acting Buprenorphine (LAB): a new form of Opioid Agonist Treatment (OAT) which is released slowly into the body to maintain treatment of opioid dependence.
- Providing Low dead space needles and syringes which reduce the amount of blood left in a needle or syringe after a liquid is injected. This innovation can significantly reduce the transmission of HIV and HCV when injecting equipment is shared.
- Community outreach on harm reduction to reduce hepatitis C among people who use stimulants and integrated hepatitis C testing and treatment in community harm reduction settings.
The project will also pilot hepatitis C testing and treatment models in a prison setting in Kyrgyzstan.
“We believe that everyone has the right to access the health services they need, including people who use drugs, and we look forward to working with Unitaid and partners to advance the integration of hepatitis C testing and treatment within harm reduction programmes,” adds Chawla.
The programme will combine the expertise of community-based organisations, regional networks, health agencies, and researchers. People who use drugs will be at the centre of designing and implementing the programme activities alongside our consortium partners, led by Frontline AIDS: Alliance for Public Health (Ukraine), Bristol University (UK), Caritas Egypt, Middle East and North Africa Harm Reduction Association (MENAHRA) (LEBANON), Education as a Vaccine (EVA) (Nigeria) and Drug Free and Preventive Healthcare Organisation (DAHPO) (Nigeria).

